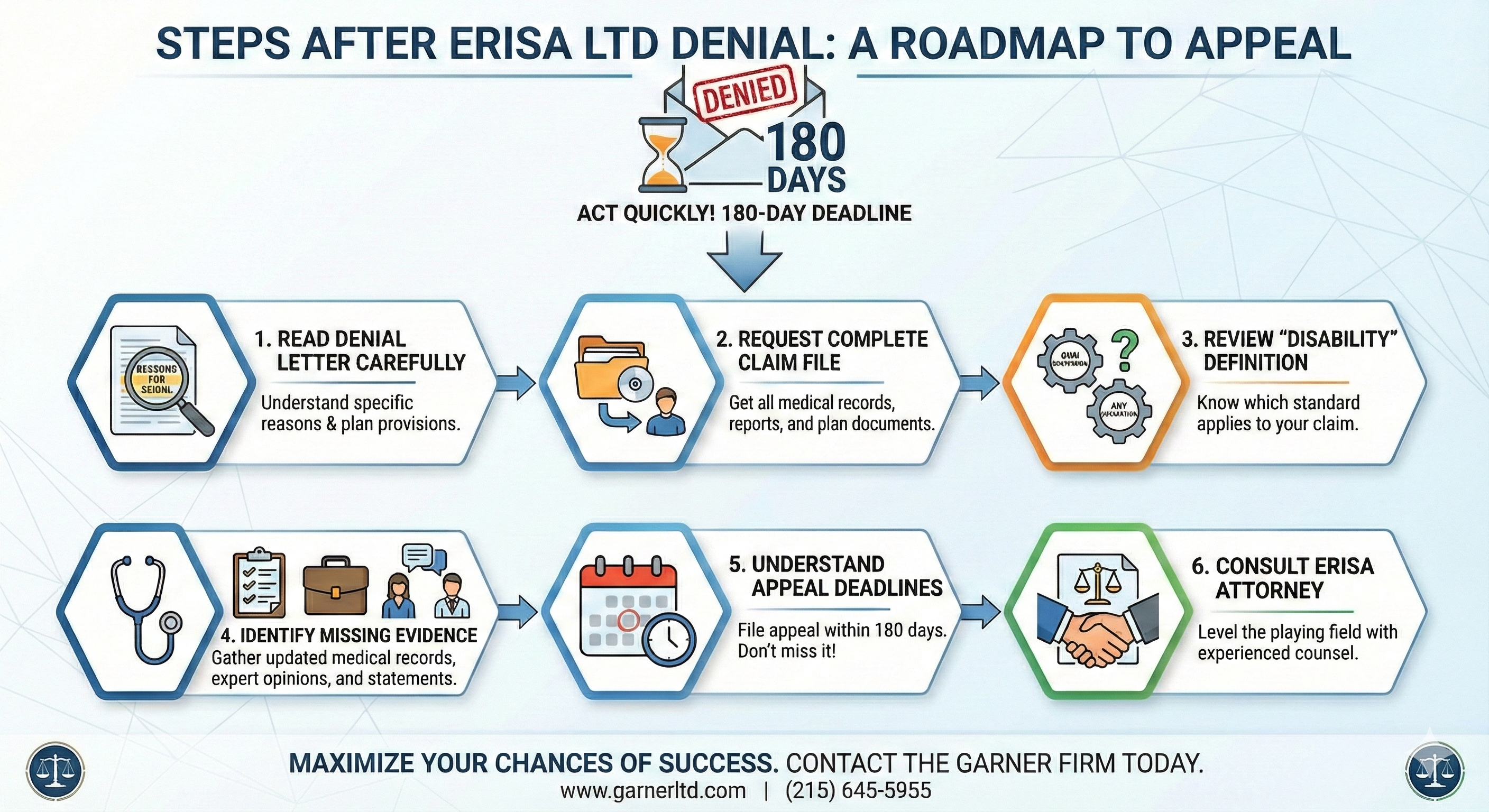
What to Do First After an ERISA Long-Term Disability Denial
Receiving a denial letter for your long-term disability (LTD) claim can be devastating. After months of medical treatment, lost income, and uncertainty about your future, the last thing you expect is for your disability insurance company to tell you that you do not qualify for benefits. If you’ve received an ERISA LTD denial, what you do next matters enormously—perhaps more than you realize.
This guide explains the critical first steps you should take immediately after receiving a denial of your LTD claim and why acting quickly and strategically can make the difference between winning and losing your benefits.
After an ERISA LTD Denial: Do Not Panic—But Do Act Quickly
The first thing to understand is that a denial of your long-term disability claim is not the end of the road. Under the Employee Retirement Income Security Act (ERISA), you have the right to appeal an adverse benefit determination. Federal regulations require that your plan provide you with a “full and fair review” of your claim, and the administrative appeal is your opportunity to challenge the denial and submit additional evidence supporting your disability.
However, time is critical. Under ERISA regulations, you have no less than 180 days from the date you receive your denial letter to file your appeal. While 180 days may seem like ample time, building a comprehensive appeal requires gathering medical records, obtaining detailed opinions from your treating physicians, and potentially engaging vocational and medical experts. Starting immediately gives you the best chance of success.
Understanding Your ERISA LTD Denial Letter
Your denial letter is a roadmap that tells you exactly why the insurance company denied your claim. Under 29 C.F.R. § 2560.503-1(g), the denial must include specific information:
- The specific reason or reasons for the denial
- Reference to the specific plan provisions on which the determination is based
- A description of any additional material or information necessary to perfect the claim
- An explanation of the plan’s review procedures and applicable time limits
- Your right to bring a civil action under ERISA Section 502(a)(1)(B) if your appeal is denied
Understanding why your claim was denied is essential to crafting a successful appeal. Common reasons for denial include insufficient medical evidence, failure to meet the plan’s definition of disability, reliance on surveillance or activity reports, or determinations that you can perform sedentary work.
Request Your Complete Claim File and Plan Documents
One of your first actions should be to request all documents relevant to your claim. Under ERISA, you are entitled to receive, upon request and free of charge, copies of all documents, records, and other information relevant to your claim. This includes:
- Your complete claim file, including all medical records reviewed
- Any surveillance videos or investigation reports
- Reports from physicians and vocational consultants retained by the insurer
- Internal emails, activity logs, and claims notes
- The plan document, summary plan description (SPD), and any applicable insurance policy
This documentation is critical because it shows you exactly what information the insurance company considered when denying your claim—and what it may have ignored or mischaracterized. Courts have criticized insurers for “cherry-picking” evidence and disregarding information favorable to claimants.
Review the Plan’s Definition of Disability
Disability insurance policies define “disability” in specific ways, and the definition that applies to your claim determines what you must prove to receive benefits. Most LTD policies use one of two standards:
Own Occupation: Benefits are payable if you cannot perform the material and substantial duties of your regular occupation—the job you were doing when you became disabled.
Any Occupation: Benefits are payable only if you cannot perform the duties of any occupation for which you are reasonably qualified by education, training, or experience.
Many policies begin with an “own occupation” standard for the first 24 months and then transition to the more restrictive “any occupation” standard. Understanding which definition applies at the time of your denial is essential because the evidence you need to submit may differ significantly depending on the standard.
Identify What Additional Evidence You Need
Based on your review of the denial letter and claim file, identify gaps in the evidence that you can fill during the appeal. A comprehensive appeal may include:
- Updated medical records: All treatment notes, diagnostic tests, imaging studies, and laboratory findings documenting your condition
- Detailed physician statements: Letters or questionnaires from your treating doctors explaining your diagnosis, functional limitations, and why you cannot work
- Functional capacity evaluation (FCE): A professional assessment of your physical abilities conducted by a qualified evaluator
- Vocational analysis: An expert opinion regarding whether jobs exist that you could perform given your limitations, education, and experience
- Social Security disability determination: If you have been awarded SSDI benefits, include the decision and supporting documentation
- Personal and lay witness statements: Declarations from you, family members, friends, and former coworkers describing how your condition affects your daily life
The administrative appeal is your best—and often only—opportunity to build the evidentiary record that will follow your case into court. In most ERISA cases, courts limit their review to the evidence contained in the administrative record.
Understand the Appeal Deadlines and Procedures
The regulations governing disability claim appeals are strict, and failure to comply with deadlines can result in losing your right to benefits. Key timelines include:
- 180 days to file your appeal from receipt of the denial;
- 45 days for the plan to issue an appeal decision, with a possible 45-day extension for special circumstances; and
- If the plan fails to issue a timely decision, your claim may be deemed denied, allowing you to proceed directly to federal court.
If you can, send your appeal well before the deadline and always use a trackable delivery method so you can prove when the plan received your submission.
Consider Consulting an Experienced ERISA Attorney
The ERISA appeal process is complex, and the stakes are high. Insurance companies have teams of claims adjusters, medical reviewers, and lawyers working to deny claims. Having an experienced ERISA disability attorney on your side can level the playing field.
At The Garner Firm, we represent individuals whose disability insurance claims have been wrongfully denied. Our attorneys have deep experience handling claims under ERISA Section 502(a)(1)(B) and understand how to build comprehensive appeals that maximize your chances of success. Firm founder Adam H. Garner has two decades of experience as an ERISA attorney and serves as Senior Editor of the treatise Employee Benefits Law.
Received an ERISA LTD Denial? Do Not Wait to Get Help
If you’ve received an ERISA LTD denial, every day counts. Contact The Garner Firm today at (267) 805-6557 or visit www.garnerltd.com to schedule a consultation with an experienced ERISA attorney. We will review your denial letter, analyze your claim file, and explain your options for pursuing the benefits you deserve.